SYDNEY CBD
SYDNEY CBD
Our stop snoring sleep doctor will go through all the anti-snoring solutions with you.


Be certain that you will get the best treatment & customer experience.
Be assured that our team of experts shall provide you with The Right Choices.
Our philosophy is a commitment to excellence in dental care & service.







Sleep Disorders are slowly being recognised as major factors in human illness and premature death.
Sleep Disorders are any condition that prohibits or affects sleep and may be medical or physiological.
This section will give you information on everything you will ever need to know about how to stop snoring & sleep apnoea, and give you appropriate solutions.
1. Dyssomnias – excessive sleepiness, the result of difficulty initiating or maintaining sleep
2. Insomnia – inability to fall asleep.
3. Parasomnia – disorders that intrudes into the normal sleep process.
4. Sleep disordered breathing – includes snoring, upper airway resistance syndrome and obstructive sleep apnoea) This is what this section talks about.
5. Sleep bruxism – grinding and clenching of your teeth

Millions suffer from sleep disorders,
which can lead to high blood pressure, heart disease and even early death. Most people with sleep disorders do not know it. And that's why you need to look into Snoring Solutions.

Sleep consists of 2 distinct states – Non REM (Rapid Eye Movement) sleep and REM Sleep.
These alternate in 90 to 110 minute cycles with a normal sleep pattern of 4 to 5 cycles.
Non REM sleep accounts for 75% of sleep and has four sequential phases.
Delta sleep is the final phase and is a deep sleep that is important for physical rest, restorative, and is characterized by large, slow delta waves in the brain.
This delta sleep accounts for a greater proportion of total sleep time in children and decreases by age 50 to 60. By 60 it is almost absent.


REM sleep improves the ability to sustain attention when awake and improves learning.
In its absence, recollection of newly learned material is impaired.
A decrease in tone of the upper airway muscles during REM sleep predisposes individuals to obstructive sleep apnoeas.
Sleep Disordered Breathing (Snoring, Upper Airway Resistance Syndrome, Obstructive Sleep Apnoea)
This is a result of an anatomical abnormality of either the oral airway or nasal passages. It is of non-psychological origin.
Oral airway problems can result from

In a person suffering from sleep disordered breathing, the airway collapses in on itself when the person breathes in and out, shutting of the airway either completely or partially.
(very important concept in the treatment for these conditions)

Snoring is often a cry for help.
Modern medicine practically ignored this nighttime distress signal until recently.
Snoring is a clear signal that an airway is blocked.
Habitual snoring often signals the presence of dangerous nighttime sleep disorders.
Sleep disorders are known to be an independent risk factor for a number of diseases, including hypertension, cardiovascular disease, cerebrovascular disease (strokes) and diabetic insulin resistance.
Snoring alone is hard on the heart and brain.
Research suggests that snorers have low night oxygen even if they do not have a sleep disorder.
Snoring has been found to be a predictor of poor school performance.
A study that compared childhood snoring at 2 to 6 years of age to school performance in middle school were more likely to have snored during early childhood.
They were also more likely to require later tonsil and adenoid removal.
Obstructive Sleep Apnoea is a complete cessation of breathing during sleep for at least 10 seconds. During an episode of OSA, the entire upper airway is blocked causing airflow to stop.
This disrupts sleep as a lack of oxygen results. The person awakens repeatedly as a result of making an effort to breathe in the presence of a lack of oxygen.

Central Sleep Apnoea is defined as a period of 10 seconds without airflow due to lack of stimulus form higher levels of the brain and the apnoea can be longer periods of time.
Mixed – Combination of the 2 above
Risk factors for sleep apnoea include obesity, increasing age, male gender, family history, alcohol, sedative use, smoking, hypertension, breathing disorders such as asthma, menopause, and anatomic abnormalities of the upper airway. A further risk factor is malocclusion (bad bite) and bruxism.

Initial evaluation is done using an Epsworth Sleepiness Scale.
Definitive diagnosis is made using an overnight sleep study called polysomnogram (PSG). The persons sleep is monitored and measured throughout the night.
Sleep Disordered Breathing is further divided in problems of nasal origin and those with oral airway problems

Snoring Surgery is helpful where there is an anatomical obstruction such as enlarged tonsils and/or adenoids, an enlarged uvula or nasal anatomical problems.
Snoring Surgery has only been found to be 30 – 50% effective
CPAP (Gold Standard of Snoring Treatment) uses a device that forms a pneumatic splint and is placed over the person’s nose during sleep.
It opens up the airway with positive pressure and has been found to be effective in moderate or severe OSA and also to stop snoring.
However compliance is very poor.
Its use is associated with laceration of the nose, rawness of the throat, bloating of the stomach, nasal congestion and ironically sleep deprivation.
(Mandibular Advancement Splints) are indicated for people with mild to moderate OSA who prefer them to CPAP (continuous positive airway pressure) therapy, or who do not respond to are not appropriate candidates for or who fail treatment attempts with CPAP as a snoring solution.
Oral appliance therapy is non invasive, less obtrusive than CPAP, and effective in the treatment of mild to moderate cases of sleep disordered breathing and to stop snoring.
Oral appliances may be worn overnight, or during t he day or both, depending on individual person’s treatment. The oral appliances are used to achieve TMJ and mandibular repositioning or tongue retention or both.
Oral appliances can sometimes cause mild discomfort and temporary minor shifts of your bite that are easily corrected by removing the appliance and by opening and closing the mouth a few times.
There are different types of oral appliances. Just like there are different shoe sizes for people, there are different appliances for sleep disordered breathing.
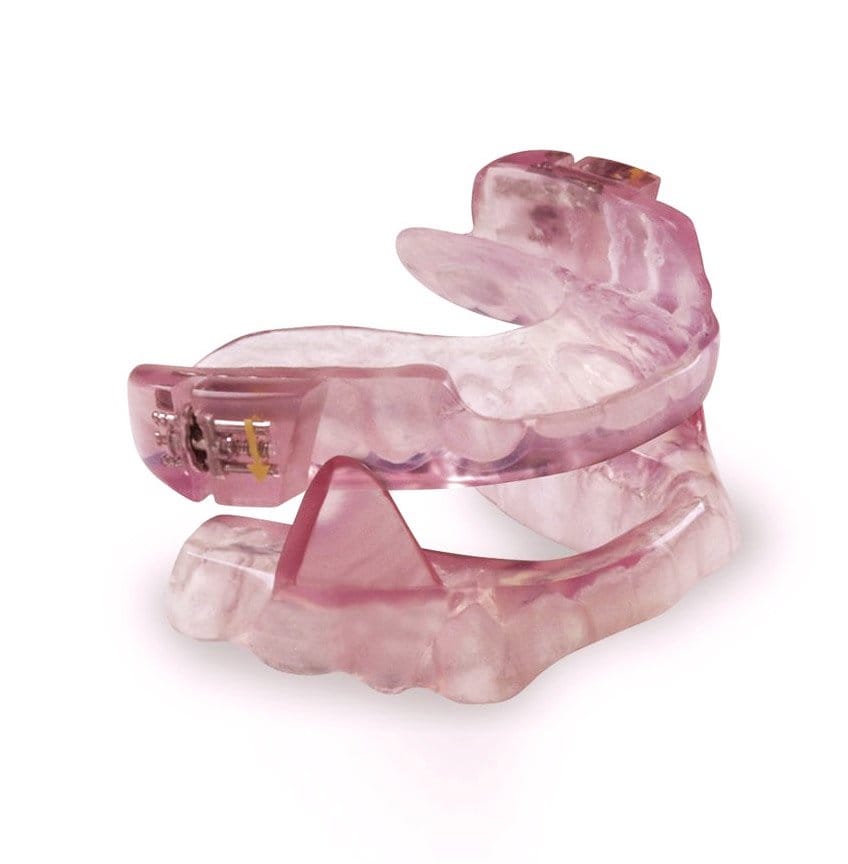

Do not get stuck into thinking of a particular brand.
Custom fabricated appliances include Silent Night, TAP, Silencer, Somnomed MAS, EMA I and II, OASYS, CPAP Pro, the tongue retaining Device and many more.
There are specific benefits to each appliance and these must be matched to each patient’s specific needs.
EXAMPLE : The SomnoMed MAS:
• Permits full range of mouth opening/closing and complete jaw closure
• Minimises disruption to normal oral functions like speech, drinking and yawning • Minimises impingement on the oral airway and the tongue space • Enables the wearer to open the mouth, yet have the jaw remain forward at all times.For additional information including published research about SomnoMed MAS a snoring solutions, please visit www.somnomed.com.au
To learn details about snoring solutions, please visit this link – https://www.tmjandsleep.com.au/snoring-sleep-apnoea/snoring.html
NightLase® Treatment is a patented, fast, non-invasive and friendly way of increasing the quality of a patient’s sleep. NightLase® lessens the effects of sleep apnea and decreases the amplitude of snoring through the use of gentle, superficial Er:YAG laser light.
No anesthesia is used in this treatment.
During NightLase® treatment laser light heats the tissue, causing tightening of the tissue which leads to an attenuation of the sound of the patients snoring and a lessening of the effects of sleep apnea.
The procedure is performed in two simple steps:
Step 1: PRECONDITIONING
The laser light preheats the tissue.
Step 2: TISSUE STRENGTHENING
Laser light strengthens the tissue.


Dr. Manish Shah is a cosmetic dentist with a special interest in porcelain veneers, dental implants and Invisalign in Sydney. He is also a medical doctor with an expertise in sleep & craniofacial pain medicine practising at Smile Concepts.
A smile can open doors and change lives.